Evidence-Based Treatment Guideline For The Management Of Lower Extremity Peripheral Artery Disease
Lower extremity peripheral artery disease occurs when plaque builds up in the arteries and slows blood flow to the legs.
You may first notice it as leg pain or tightness when walking. Over time, though, the symptoms can become more noticeable. And in the most advanced stages, symptoms may appear even at rest.
It’s important to get the basic guidelines for the management of lower extremity peripheral artery disease immediately after diagnosis.
Treatment is not limited to one solution. And it usually involves a combination of lifestyle changes, medications, and structured exercises. In some cases, more intensive medical procedures may be required to improve blood flow.
The right approach depends on how advanced the condition is and what symptoms are present. Some need help controlling risk factors early on. Others need treatments that are aimed at improving mobility or preventing complications.
We are going to walk you through the most effective ways to manage PAD as recommended by healthcare experts.
Guideline For The Management Of Lower Extremity Peripheral Artery Disease
Managing lower extremity PAD follows a stepwise approach. The goal here is to improve blood flow to the legs, reduce symptoms, and lower the risk of cardiovascular events.
Healthcare professionals decide treatments based on the severity of symptoms, functional limitations, and the overall vascular risk.
In most cases, patients have to start with conservative treatments. These treatments address the underlying cause of PAD, and they form the foundation of long-term care.
You would be asked to continue these even after additional measures are introduced to your overall treatment plan.
Understanding how each component fits into the overall management of lower extremity peripheral arterial disease can help set realistic expectations.
Lifestyle And Risk Factor Modification
This is the cornerstone of PAD management. If you don’t address these factors, symptoms can get worse, and other treatment options may fail to produce the desired results.
The most critical thing is to stop smoking. Smoking accelerates the damage that occurs in your arteries and worsens the symptoms. It also significantly increases the risk of heart attack and stroke.
Even long-term smokers see measurable improvements after quitting.
Controlling blood pressure, cholesterol, and blood sugar is also equally important. Hypertension and dyslipidemia contribute directly to plaque buildup. Diabetes increases both the severity of PAD diseases and the risk of non-healing wounds.
Dietary changes, weight management, and regular physical activity support the overall treatment plan and also reduce cardiovascular risk.
Guideline-Directed Medical Therapy
Medications play a central role in PAD treatment, as they protect you against systemic complications. Antiplatelet therapy is commonly prescribed to reduce the risk of clot formation.
Statin therapy is recommended for most patients regardless of baseline cholesterol levels. That’s because these play a role in stabilizing plaque and slowing the progression of the disease.
The doctors may also prescribe medications to lower blood pressure. In the case of some patients, doctors may consider antithrombotic therapy to further reduce cardiovascular and limb-related events.
Together, these medications form the foundation of treatment. And patients are typically asked to continue with the medications even when symptoms improve.

Structured Exercise Therapy
PAD patients who struggle to walk due to the symptoms greatly benefit from structured exercise therapy. It works by making the muscles more efficient. It helps develop collateral circulation and improve overall cardiovascular health.
Supervised exercise programs, in particular, have shown consistent benefits. Gradually, the pain while walking eases, and patients can walk longer distances without having to rest.
These programs usually involve walking to the point of moderate discomfort. Then, patients can rest until symptoms disappear. Start walking again. They need to repeat this cycle to see results over time.
When supervised programs are not accessible, structured home exercises with guidance and monitoring can also work.
Just remember that exercise is not a replacement for medical therapy. It complements it and often determines what level of functional improvements you’ll see.
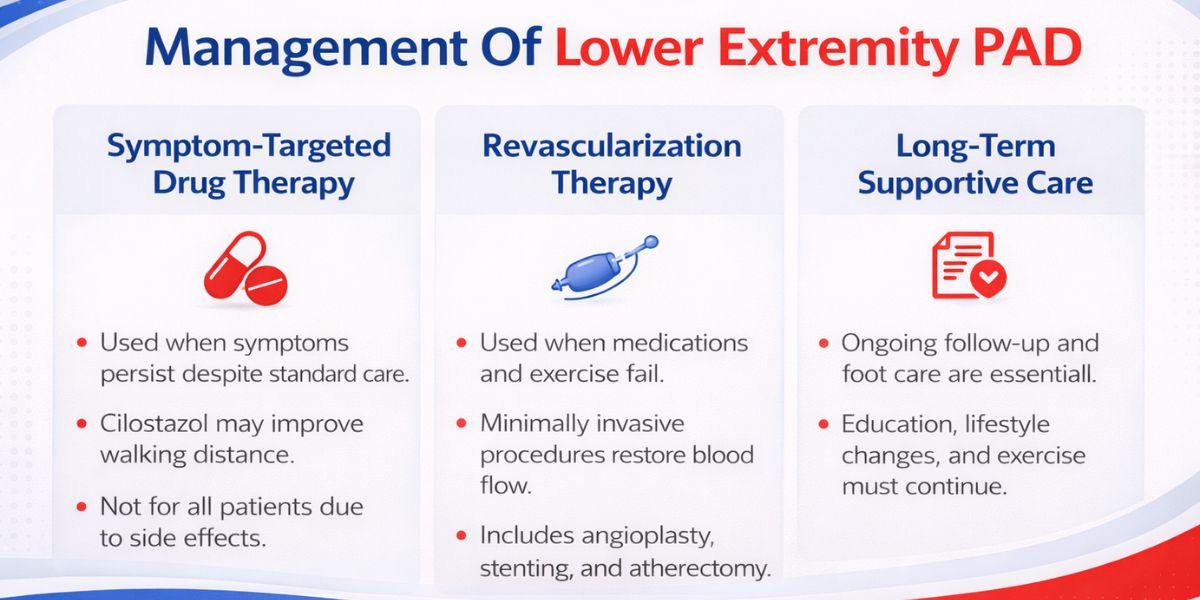
Symptom-Targeted Pharmacologic Therapies
Some patients continue to experience functional limitations even after controlling risk factors, exercising regularly, and taking their medications.
In such cases, doctors may recommend symptom-targeted pharmacologic therapies. These agents don’t replace the foundational therapies. But they can reduce the symptoms more effectively in some patients.
Cilostazol is the most commonly used medication for this purpose. It’s known to help patients who experience intermittent claudication walk longer distances without pain.
However, its use is limited because of the associated side effects. Heart failure, headaches, and palpitations are the most common of these side effects.
Other medications have also been studied, but they all show limited or inconsistent benefits. That’s why they are not routinely recommended for the management of lower extremity PAD.
Revascularization Therapies For Lower Extremity PAD
Revascularization is needed when conservative treatment methods and structured exercises fail to produce any desirable results.
The goal of revascularization is to restore blood flow, reduce ischemic PAD symptoms, and prevent tissue loss. These therapies are considered part of comprehensive PAD management. They cannot entirely replace medical treatment.
Endovascular approaches are commonly used, as they are minimally invasive. Balloon angioplasty and stenting can widen the narrowed arteries and thereby improve circulation.
Laser atherectomy, also referred to as laser ablation, uses laser energy to remove atherosclerotic plaque from the arterial wall. It is often used in complex or calcified lesions. It’s also often combined with angioplasty or stenting. Doctors choose a revascularization approach based on how severe the condition is and the overall patient risk.
Supportive Strategies For Long-Term Management
Long-term management of lower extremity peripheral artery disease extends beyond simply relieving symptoms. Ongoing care focuses on preventing complications and maintaining functional independence.
Foot care is especially important for patients with diabetes or reduced sensation. Small injuries can progress quickly when circulation is impaired.
Regular follow-ups allow doctors to reassess symptoms, monitor treatment response, and adjust therapies as needed. Educating the patient also plays a key role.
Understanding the chronic nature of PAD helps patients understand why they need to keep taking the medications, exercise regularly, and stick to the lifestyle changes.
Choosing The Right Care Team For The Management Of Lower Extremities PAD
As you know by now, managing this condition effectively requires careful evaluation, constant modifications, and ongoing follow-up. How well the treatments and therapies work depends entirely on how methodically they are planned for your specific case.
That’s why you should always rely on a reliable clinic like the Advanced Medical Group. Here, we bring together experienced PAD specialists, diagnostic capabilities, and modern treatment options, including minimally invasive therapies.
Contact us today to get access to a comprehensive care team that can create the best treatment plan for you.