Managing PAD With The Right Daily Habits For Long-Term Circulation Health
The conversation usually goes one of two ways. Either your doctor tells you peripheral artery disease runs in the family and there’s not much to do about it, or they hand you a prescription and move on to the next patient. Neither is the full story.
Managing PAD starts earlier than either version suggests. Not at the pharmacy counter. Not in an operating room. In your kitchen. On your walk. In the habits you repeat every day, even when nobody’s watching.
These habits don’t replace medical care. They’re the foundation everything else stands on. For many patients, the difference between slow, stable PAD and a fast-progressing one comes down to what you do every day. The good news? None of these habits require expensive equipment or a complete life overhaul. They just require repetition.
Daily Habits That Make A Real Difference In Managing PAD
Here’s what most people miss — it’s not any one habit that turns things around. It’s the combination. Six small, consistent choices working together. Each one reinforces the others, and none of them works as well alone.
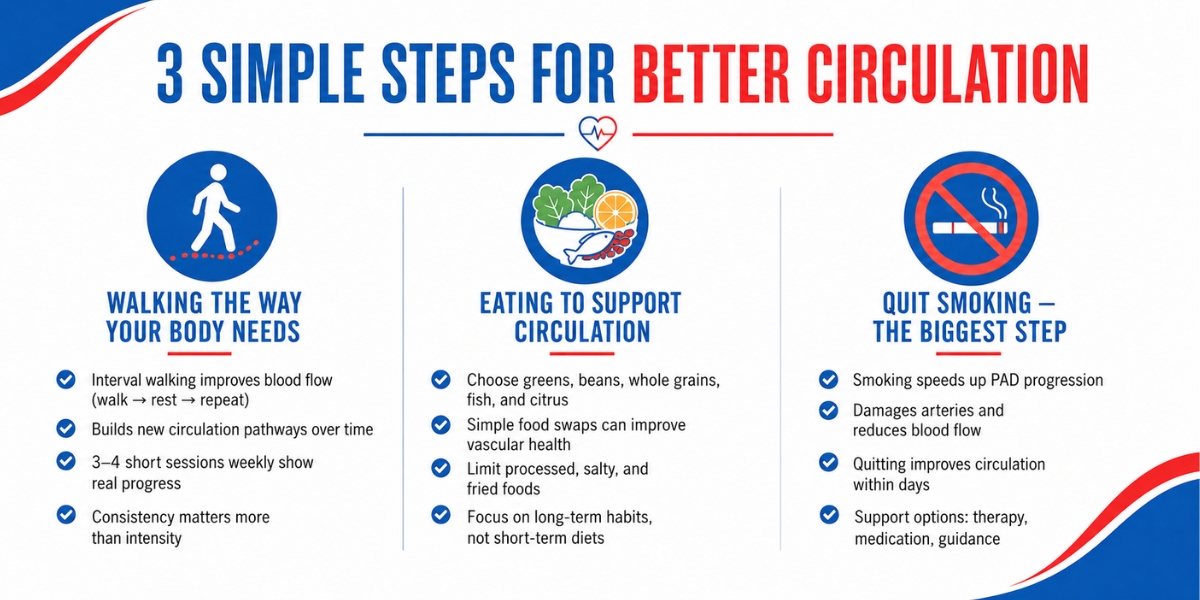
Walking The Way Your Body Actually Needs It
Walking is the treatment most patients don’t expect — and the one that takes the most grit. When your legs cramp and you keep going, rest, and start moving again, your body slowly builds new pathways for blood flow. Vascular specialists call this collateral circulation.
This isn’t about long strolls or hitting a step count. Clinical research supports structured interval walking — go until the ache starts, stop and rest, go again. Three or four short sessions a week is enough to start, and most patients notice improvement in walking distance within a few weeks.
Consistency beats intensity every time. Managing PAD through healthy daily habits starts with movement — but the kind of movement your body can sustain, not the kind that leaves you sore the next day.
Eating To Support Circulation
You don’t need to overhaul your kitchen. A few swaps go a long way.
Leafy greens, beans, lentils, citrus fruits, whole grains, and fish all support vascular health. These are foods healthcare professionals recommend for anyone living with circulation issues — and most of them are already stocked in grocery stores across Hudson County.
What to quietly push off the plate? Salt-heavy processed foods, cured meats, and fried items. These stress blood vessels in ways that work directly against what you’re building.
Think of food as one of the right daily habits to manage PAD — not a diet to follow for three weeks, but a pattern you can live with for years.
Quitting Smoking: The Single Biggest Thing You Can Do
If you smoke, this is the habit that matters most. Full stop.
Smoking accelerates PAD disease faster than almost anything else. It damages artery walls, narrows blood vessels, and undoes the benefits of everything else you’re doing — the walking, the eating, the medication.
Quitting is hard. Nobody pretends otherwise. But you don’t have to lean on willpower alone. Nicotine replacement, counseling, and prescription medications have all been shown to help. Your doctor can walk you through the options that fit your situation.
Even partial progress matters. The arteries begin responding within days of your last cigarette.
Taking Your Medications Like Clockwork
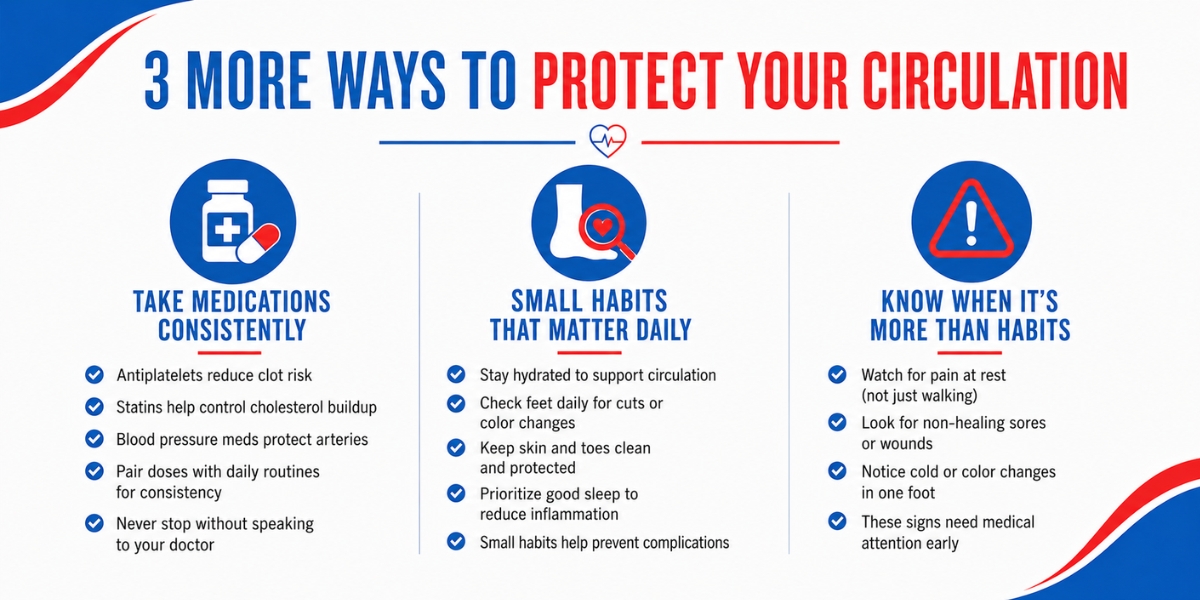
If your doctor prescribed antiplatelet medications, statins, or blood pressure drugs, these aren’t optional. They work in the background — quietly stabilizing the conditions that caused PAD disease in the first place. Antiplatelets reduce clotting risk. Statins help manage the cholesterol that fuels plaque. Blood pressure medications protect artery walls from ongoing stress.
The trick with consistency isn’t motivation. It’s pairing. Link your pill to something you already do every day. Morning coffee. Brushing your teeth. Feeding the dog.
And if you’re having side effects, say so. Don’t stop silently. PAD treatment only works when it’s ongoing, and your doctor can adjust the plan — but only if they know.
Small Habits That Compound: Hydration, Foot Care, Sleep
These are the ones people skip. They shouldn’t.
Hydration thins the blood and supports smoother circulation. Most adults don’t drink enough — especially in the evening when they’re trying to avoid waking up thirsty.
Daily foot care is non-negotiable. Check your feet once a day for cuts, blisters, color changes, or patches that haven’t healed. Look at the soles. Look between the toes. These are early PAD symptoms that deserve attention before they turn into something worse — especially when nerve sensitivity is reduced and small injuries are easy to miss.
And sleep matters more than people realize. Chronic sleep loss raises blood pressure and inflammation — two things you can’t afford to stack on top of vascular disease.
Recognizing When Daily Habits Aren’t Enough
Here’s the part nobody talks about. Sometimes the habits do everything they can — and the condition still progresses.
Watch for rest pain. Pain that shows up when you’re sitting or lying down, not just when you walk. Watch for sores or cuts on the lower legs that aren’t healing. Watch for sudden coldness or a dramatic color change in one foot compared to the other.
These are signals that peripheral artery disease has moved past the point where lifestyle alone can manage it. They’re not a failure — they’re information. Catching them early gives you more treatment options, not fewer.
The Habits Stack, And The Care Team Stays Close
Managing PAD isn’t about doing any one thing perfectly. It’s about showing up every day, in small ways, and having a team you can call when something shifts.
Managing PAD with the right daily habits is the quiet, consistent work. But you’re not doing it alone. Advanced Medical Group helps patients build practical PAD management plans — combining lifestyle guidance, medication support, and monitoring for when the picture changes. If you’ve been diagnosed with PAD and want clarity on where you stand, a vascular evaluation is the most useful first step.