Which Blood Test For PAD Do Most Experienced Doctors Recommend?
Have you been noticing leg pain or cramping when you walk? Does it get better when you rest? Do wounds on your feet seem to heal slowly? If you’ve answered yes to all of them, it may be smart to get a blood test for PAD.
These are some of the more common signs doctors look for when evaluating peripheral artery disease, or PAD for short.
It is a condition where the arteries in the legs get narrowed due to plaque buildup. That reduces blood flow to the legs. And that’s what causes your legs to hurt when you walk or move around.
However, there’s one thing you should know from the start. Blood tests alone cannot diagnose PAD.
Blood tests are the first step in the diagnosis process. Most doctors order them because they provide critical background information on the patient.
Blood tests also help uncover other conditions that may have contributed to PAD. However, blood tests cannot identify where the artery is narrowed or how severe the blockage is. That’s why follow-up tests are required.
Having said that, it’s important to know which blood tests are usually ordered for PAD if you suspect this diagnosis.
The Most Common Blood Test For PAD
The first thing you should know is that there is no single blood test that can conclusively tell you whether you have PAD. There are, however, several blood tests for PAD that help in the initial diagnosis.
PAD usually doesn’t happen in isolation. In most cases, there are common signs in the body that indicate whether an artery-related disorder may be present.
That’s why the blood tests are ordered. The goal is to see what might have caused PAD in the first place. But since blood tests alone cannot identify the blocked artery, several other tests are required.
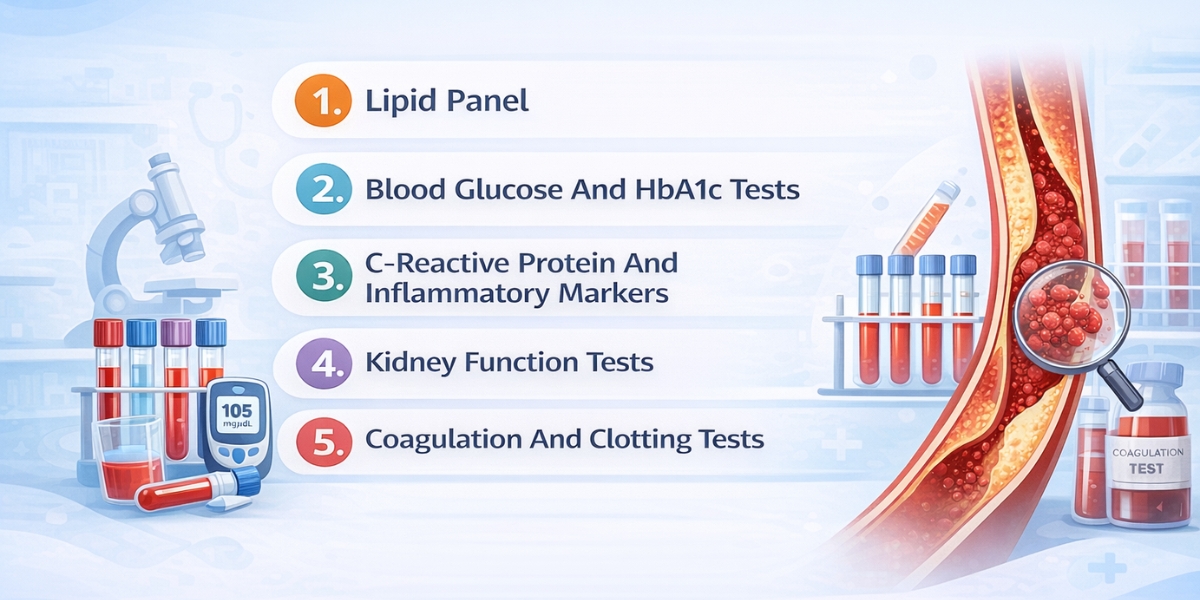
1. Lipid Panel:
You may know it as the cholesterol test. A lipid panel measures different types of cholesterol and fats in the blood. The ones that doctors want to check are LDL or “bad” cholesterol, HDL or “good” cholesterol, total cholesterol, and triglycerides.
These values matter because peripheral artery disease is most often caused by atherosclerosis. It is a process in which fatty deposits build up inside the artery walls, gradually blocking it.
Elevated LDL cholesterol is particularly important in PAD. Over time, excess LDL is what causes plaque to build up inside the arteries. Triglycerides can also play a role, especially in people with diabetes or metabolic syndrome.
HDL helps transport cholesterol away from the arteries. That is why lower HDL levels are associated with higher vascular risk.
With the lipid panel test, doctors can tell how active the atherosclerotic process may be. Based on this, they may or may not prescribe medication to lower cholesterol.
2. Blood Glucose And HbA1c Tests:
These tests tell you how well your body is regulating blood sugar. A glucose test reflects the blood sugar level at a single point in time. HbA1c shows the average blood sugar level over the past two to three months.
HbA1c is often more informative because it captures long-term patterns rather than day-to-day fluctuations.
Diabetes is one of the strongest risk factors for peripheral artery disease. If blood sugar stays consistently high, the inner lining of the blood vessels gets damaged. And such damaged blood vessels are more prone to plaque buildup.
Diabetes also affects small blood vessels. This can worsen circulation in the feet. That’s why people who have both PAD and diabetes are at a higher risk for developing ulcers and infections.
3. C-Reactive Protein And Inflammatory Markers:
C-reactive protein is often measured as high-sensitivity CRP, or hs-CRP. It is a blood marker of inflammation. But what is inflammation, exactly?
It is the body’s immune response, and it can become chronically active in certain conditions, including atherosclerosis. An elevated hs-CRP does not point to a specific artery problem. But it does suggest that there’s inflammation in the body, and it is likely affecting the vascular system.
Inflammation plays a key role in how plaques develop within arteries. Inflamed plaques are more likely to grow, become unstable, and worsen PAD symptoms.
In people with PAD, higher inflammatory markers are associated with increased cardiovascular risk, even when cholesterol levels are not severely elevated.
But it is extremely important to interpret CRP carefully. Levels can rise due to infections, injuries, or other inflammatory conditions that are unrelated to PAD.
4. Kidney Function Tests:
These are the creatinine and eGFR tests. Creatinine is a waste product filtered out by the kidneys. And eGFR is a calculated value that estimates how efficiently the kidneys are doing that job. Together, these tests give a practical picture of overall kidney health.
Kidney disease and PAD often go hand in hand. Both of these are linked to long-standing conditions like diabetes, high blood pressure, and atherosclerosis.
When the kidneys stop functioning properly, the risk of vascular disease increases. The combination of the two also causes circulation issues in smaller blood vessels.
But kidney tests serve a bigger function than just PAD diagnosis. Doctors need to determine how well your kidneys function to determine which medications to prescribe for PAD treatment.
5. Coagulation And Clotting Tests:
Coagulation and clotting tests assess how the blood forms clots. The tests also show how well that process is regulated.
Common tests include platelet counts, prothrombin time, and activated partial thromboplastin time. Platelets are blood cells that help stop bleeding. PT and aPTT measure how long it takes blood to clot through different pathways.
Someone with PAD already suffers from poor blood flow due to narrowed arteries. If there’s abnormal clotting on top of that, the risk of sudden blockage increases.
However, doctors don’t order the clotting tests for everyone. They only recommend it for those who are at high risk for acute limb ischemia. In such cases, they may prescribe blood-thinning medications.
By now, the answer to the question “What blood test is done for PAD?” should be clear to you. Just remember that additional tests will be required for a final diagnosis.
Getting The Right Diagnosis And Treatment For PAD
Getting an accurate diagnosis for PAD starts with knowing what each test can and cannot tell you. We’ve already discussed why blood tests are needed and why they aren’t the only tests you will need.
Once the diagnosis is final, it’s time to start treatment. Advanced Medical Group takes a methodical and comprehensive approach to PAD treatment.
Our doctors first do all the necessary tests to diagnose PAD and understand what might be causing it. They will then formulate a treatment plan that’s specifically for you.