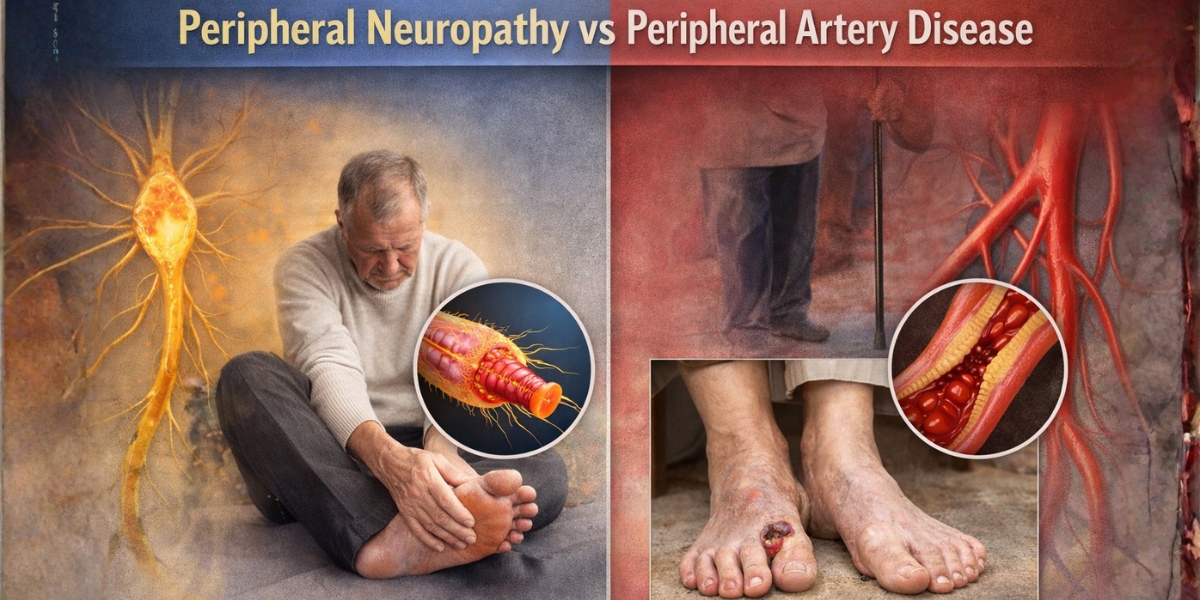
Key Differences And Health Impacts Of Peripheral Neuropathy vs Peripheral Artery Disease
Have you been experiencing pain, numbness, tingling, or weakness in the legs? If so, your first instinct might be to do a quick Google search for it.
If you do that, you are likely to come across two medical conditions called peripheral neuropathy and peripheral artery disease. Both conditions affect similar areas of the body, particularly the legs and feet. And some of their symptoms appear similar at first.
However, despite the surface similarities, these are two fundamentally different conditions. Without a clear understanding of peripheral neuropathy vs peripheral artery disease, it’s easy to be confused.
Peripheral neuropathy involves damage to the nerves. It affects how signals are sent and received. Peripheral artery disease is a circulatory disorder. It occurs when plaque builds up in the arteries and reduces blood flow.
Since the underlying problem is different, how each condition is diagnosed and treated also varies significantly.
Peripheral Neuropathy vs Peripheral Artery Disease Differences
Because of their overlapping symptoms, people, even healthcare professionals, often initially misdiagnose PAD for peripheral neuropathy or vice versa.
It’s also crucial to understand how these two conditions differ to avoid any confusion. So, here, we’ll give you an overview of peripheral artery disease vs peripheral neuropathy.
1. Underlying Disease
Peripheral artery disease and peripheral neuropathy affect different systems. And this difference affects how and what symptoms appear and what PAD treatment is pursued.
Peripheral Artery Disease:
Also called PAD, peripheral artery disease occurs because of the narrowing or blockage of the arteries that supply blood to the legs. It happens due to atherosclerosis, which is when fatty deposits build up inside the artery walls.
Over time, this limits blood flow. When this happens, muscles get tired quickly during activity. In advanced stages of the condition, muscle fatigue and pain may occur even at rest.
Peripheral Neuropathy:
Peripheral neuropathy occurs when the nerves outside the brain and spinal cord, also known as peripheral nerves, are damaged. These nerves carry signals related to sensation, movement, and automatic functions like temperature control or sweating.
When they get damaged, these signals may be delayed, distorted, or lost altogether. That’s why peripheral neuropathy often produces abnormal sensations. It doesn’t necessarily cause pain during physical exertion.
2. Physical Changes In The Legs And Feet
A physical examination may also reveal signs of one or the other condition.
Peripheral Artery Disease:
PAD can cause visible and measurable changes in the legs and feet. Skin may appear pale or bluish. It may feel cool to the touch or become thin and shiny over time.
Hair growth on the legs may decrease. Pulses in the feet may be weak or absent, reflecting reduced blood flow. Cuts or sores may heal slowly, or not at all, due to inadequate circulation.
Peripheral Neuropathy:
In neuropathy, the skin often appears normal, but sensation is altered. You may not feel temperature changes, pressure, or pain as expected.
Muscle weakness and balance issues can develop. It happens especially if the motor nerves get damaged.

3. Signs and Symptoms
On the surface, some PAD symptoms may appear similar to those of neuropathy. That’s what often causes people to confuse the two conditions.
Peripheral Artery Disease:
The symptoms associated with PAD are caused by reduced blood flow. The most common symptom is leg pain or cramping that occurs when walking and eases when resting. This pattern is also known as intermittent claudication.
Other common symptoms of PAD are a feeling of heaviness in the legs, coldness in the feet, changes in skin color, or wounds that heal slowly due to poor circulation.
Peripheral Neuropathy:
Neuropathy symptoms are more sensory in nature and not based on activity. That’s the main takeaway in the differences of symptoms in PAD vs neuropathy.
Those with this condition may experience tingling, burning, or stabbing sensations. A lack of sensation or numbness is also a symptom. These symptoms often worsen at night and may persist even when resting.
Because of the impaired sensations, afflicted individuals may not realize when there’s a minor injury in the area. That becomes a problem over time.
4. Pattern And Timing Of Pain
When discussing the symptoms, it’s just as important to talk about when these symptoms appear.
Peripheral Artery Disease:
The pain associated with PAD usually follows a predictable pattern. It typically develops during physical activity such as walking or climbing stairs. The pain goes away after a short period of rest.
It happens because the muscles in the area require more oxygen during activity. And they don’t get that because of the poor blood flow. When circulation catches up while resting, the pain subsides.
In more advanced stages of PAD, pain may appear even during inactivity. That indicates a more severe blood flow issue.
Peripheral Neuropathy:
Neuropathic pain does not depend on the level of activity. It may appear suddenly, linger without a clear trigger, or worsen during periods of inactivity. The pain may get worse at night.
It happens when the damaged nerves misfire or cannot regulate sensory signals properly.
5. Risk Factors And Triggers
Both conditions share some risk factors. But how those risks affect the body is significantly different in peripheral artery disease vs neuropathy.
Peripheral Artery Disease:
Everything that can damage the blood vessels over time is a risk factor for PAD. Smoking, high cholesterol, high blood pressure, and aging can all contribute to the narrowing of the arteries.
Diabetes can also accelerate vascular damage. It makes arteries stiffer and more prone to plaque buildup. A sedentary lifestyle can further compound these effects by reducing the overall efficiency of blood circulation.
Peripheral Neuropathy:
Anything that can damage the peripheral nerves is a risk factor for neuropathy. Diabetes is again a major contributor. However, in this case, the elevated blood sugar levels damage nerve fibres.
Chronic alcohol use, vitamin deficiencies, autoimmune disorders, and infections are also common triggers. It may even be caused as a side effect of certain medications.
6. Diagnostic Evaluation
To get an accurate diagnosis, a doctor will prescribe specific tests. These tests produce results that are not interchangeable.
Peripheral Artery Disease:
To diagnose PAD, doctors focus on blood flow. A common test is the ankle-brachial index. It compares the blood pressure in the ankle to the blood pressure in the arm.
Lower readings in the ankle indicate poor blood flow to the legs. A doctor may also prescribe imaging studies such as a vascular ultrasound or angiography.
It is necessary to visualize the narrowing or blocked arteries and how severe the condition is.
Peripheral Neuropathy:
To detect neuropathy, a doctor may prescribe nerve conduction studies. The test measures how quickly electrical signals travel through the nerves. Slowed or weakened signals could mean nerve damage.
Electromyography is another common test. It evaluates how muscles respond to nerve signals.

Finding The Right Treatment For Both Conditions
After getting an accurate diagnosis, it’s necessary to get on the best treatment plan. Since the treatment for each condition varies wildly, you must seek experts.
At Advanced Medical Group, you will find the best treatment for PAD. With decades of experience under their belt, the doctors here successfully treat PAD.